The provision of programs to prevent the spread of HIV and hepatitis among people who inject drugs
(PWID) is inadequate in many countries around the world and presents a critical public health
problem, comprehensive reviews by Australian researchers from the National Drug and Alcohol
Research Centre at UNSW have found.
The two reviews of the global prevalence of injecting drug use and of interventions to prevent the
spread of blood borne viruses among people who inject drugs are published today in leading
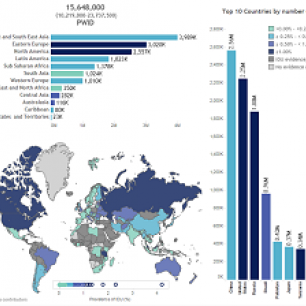
international journal The Lancet Global Health. The authors estimate that 15.6 million people have
recently injected drugs. Of these, 18 per cent are living with HIV infection and 52 per cent test positive
for hepatitis C antibody.
Yet despite evidence that needle and syringe programs (NSP) and opioid substitution therapy (OST)
reduce HIV and HCV infections, they are still not being implemented in many places, and few people
can access them in many countries, the authors found.
Australia is one of only four countries worldwide with high coverage of both NSP and OST – the
others are Austria, the Netherlands and Norway. In Australasia 1.1 per cent of PWID are living with
HIV compared with 25 per cent of PWID in Eastern Europe, 36 per cent in Latin America, 18 per cent
in Sub Saharan Africa and 19 per cent in South Asia. By contrast, the prevalence of hepatitis C
among PWID is more evenly spread – 57 per cent of the people who inject drugs in Australia and
New Zealand test positive for hepatitis C antibodies, compared with 64 per cent in Central Europe, 55
per cent in North America and 50 per cent in East and South-East Asia.
“Across all countries a substantial number of people who inject drugs are living with HIV or HCV and
are exposed to multiple adverse risk environments that increase health harms,” says UNSW’s
Professor Louisa Degenhardt, lead author of the paper reviewing prevalence of injecting drug use and
HIV and Hepatitis in this population.
The reviews of global prevalence of injecting drug use and of provision of programs to prevent the
spread of blood borne viruses is the first to be conducted since 2008, although the results are not
directly comparable due to different and more sophisticated data collection techniques, and better
country specific record keeping. Evidence of injecting drug use was found in an additional 33
countries compared with the last review – predominantly from Sub Saharan Africa.
Just over half (52 per cent) of the countries with evidence of injecting drug use had needle syringe
programs and medical treatment to encourage reductions in injecting – opioid substitution therapy –
was available in less than half of all countries identified (48 per cent).
“Coverage of HIV and HCV prevention interventions for PWID remains poor and is likely to be
insufficient to effectively prevent HIV and HCV transmission. Scaling up of interventions for PWID
remains a crucial priority for halting the HIV and HCV epidemics,” says UNSW’s Dr Sarah Larney,
lead author of the paper on global coverage of interventions.
“The presence of interventions alone is not sufficient; the greatest prevention benefits are reported
when NSP and OST are implemented in high coverage and in combination,” Dr Larney adds.
The three regions worldwide with the highest populations of people who inject drugs, east and southeast
Asia, Eastern Europe and North America, all had poor provision of needle syringe programs and
opioid substitution therapy. HIV prevalence in these countries was high ranging from 9 per cent in
North America to 25 per cent in Eastern Europe. By contrast, only one per cent of people who inject
drugs in Australia and New Zealand are living with HIV.
“Several countries in these regions have experienced recent HIV outbreaks as well as persistently
high HCV prevalence among PWID,” write the authors.
For example, Russia, which has almost 2 million people who inject drugs, nearly 30 per cent of whom
have HIV and 69 per cent of whom have hepatitis C, does not provide OST and has very limited
access to NSP, the authors found.
Media contacts:
Marion Downey
Communications Manager, National Drug and Alcohol Research Centre
P: (02) 9385 0180 | 0401 713 850 | m.downey@unsw.edu.au
Morgaine Wallace-Steele
Communications Officer, National Drug and Alcohol Research Centre
P: (02) 9385 0124 | 0432 894 776 | m.wallace-steele@unsw.edu.au
Degenhardt, L., Peacock, A., Colledge, S., Leung, J., Grebely, J., Vickerman, P., Stone, J.,
Cunningham, E.B., Trickey, A., Dumchev, K., Lynskey, M., Griffiths, P., Mattick, R.P., Hickman, M.,
Larney, S. (2017). Global prevalence of injecting drug use and sociodemographic characteristics and
prevalence of HIV, HBV, and HCV in people who inject drugs: a multistage systematic review. Lancet
Global Health, published online October 23 2017.
- To access this journal article please visit The Lancet Global Health.
- Interactive dashboards containing data from this study are available on the NDARC website.
Larney, S., Peacock, A., Leung, J., Colledge, S., Hickman, M., Vickerman, P., Grebely, J., Dumchev,
K., Griffiths, P., Hines, L., Cunningham, E.B., Mattick, R.P., Lynskey, M., Marsden, J., Strang, J.,
Degenhardt, L. Global, regional, and country-level coverage of interventions to prevent and manage
HIV and hepatitis C among people who inject drugs: A systematic review. Lancet Global Health,
published online October 23 2017.
- To access the journal article please visit The Lancet Global Health.
- Interactive dashboards containing data from this study are available on the NDARC website.