Dr Sonu Bhaskar was awarded $40,000 in the 2017 round of UNSW Medicine Neuroscience, Mental Health and Addiction Theme and SPHERE Clinical Academic Group (CAG) Collaborative Research Seed Funding for the project, Thrombolysis and Endovascular WorkFLOw Network (TEFLON) trial.

Name: Dr Sonu Bhaskar
Position/s:
Neurovascular Fellow (Stroke/Neurology), Department of Neurology and Neurophysiology, Liverpool Hospital, Sydney
Executive Officer, Deputy Vice-Chancellor (DVC) Enterprise/Maridulu Budyari Gumal - The Sydney Partnership for Health, Education, Research and Enterprise (SPHERE), The University of New South Wales (UNSW)
Team Lead, Neurovascular Imaging Lab, Clinical Sciences Stream, Ingham Institute for Applied Medical Research, Liverpool
How has the Neuroscience, Mental Health and Addiction Theme and CAG enabled you to develop your research interests?
The seed funding has acted as a “springboard” in developing my clinical and academic leadership/research profile by helping me develop, optimise and embed acute stroke reperfusion therapy workflow as a part of the Thrombolysis and Endovascular WorkFLOw Network (TEFLON) trial. The provision of this grant has allowed me to engage with various stakeholders cutting across departments within hospitals, local health districts (LHD) and universities and build my skills in developing health systems improvement-based intervention package and associated clinical trial design and mobilizing support from various stakeholders with a view to translating the intervention package into a health policy.
To this end, I have been fortunate to work closely with senior executives in South Western Sydney Local Health District (SWSLHD), Liverpool Hospital and Ingham Institute; senior clinicians and various bodies including NSW Ambulance in the co-design, implementation and roll-out of the TEFLON intervention. This has allowed me to gain skills in stroke care implementation pathways. Overall, this has been a learning and engaging experience and provided me with an opportunity to build a strong track record in implementation science, systems change and clinical leadership.
Every clinical and research endeavor is teamwork, and I am very proud of an incredibly awesome team we have at Liverpool led by Dr Alan McDougall who has been critical in giving me the opportunity and support that a project like this entails. The invaluable support from the SWSLHD Neuroscience Data Management Team led by Dr Peter Thomas and our nursing staff led by CNC Angela Firtko has been critical in steering a project of this scale.
I am also very grateful for the sponsorship and support I have received from my mentors and Senior Clinicians like Prof Les Bokey (SWSLHD), Prof Christopher Levi (SPHERE), Dr Alan McDougall (Neurology and Neurophysiology/Liverpool Hospital), A/Prof Dennis Cordato (Neurophysiology/Liverpool Hospital), Dr Cecilia Cappelen-Smith (Neurophysiology/Liverpool Hospital), A/Prof Suzanne Hodgkinson (Neurology/Liverpool Hospital), A/Prof Alessandro Zagami (Neurology/Prince of Wales Hospital), Dr Jason Wenderoth (Interventional Neuroradiology/Liverpool & Prince of Wales Hospitals), Dr Andrew Cheung (Interventional Neuroradiology/Liverpool & Prince of Wales Hospitals) and A/Prof Paul Middleton (Emergency Medicine/Liverpool Hospital).
In parallel to this, I am humbled and fortunate to lead and establish an Australia-first initiative NSW Brain Clot Bank with A/Prof Murray Killingsworth. NSW Brain Clot Bank has been recently successful in securing four year substantial funding from the NSW Ministry of Health. This grant will enable the establishment of a NSW collection for thrombectomy samples (retrieved after endovascular thrombectomy following an acute ischemic stroke) to be housed at the NSW State-wide Biobank Facility and harmonise clot collection, storage and processing workflow across NSW Health Pathology network.
It has been an incredible journey of learning, sharing and creating (new) knowledge with an overarching goal to improve patient outcomes.
Your project, Thrombolysis and Endovascular WorkFLOw Network (TEFLON) Trial was successful in the 2017 round of Theme and CAG collaborative research seed funding. Can you please tell us about the project?
There is a pressing need to identify effective strategies for changing a range of health care practices, especially unwarranted variations in clinical care or process parameters. We have best-evidence for reperfusion therapy, including endovascular thrombectomy (EVT) and/or systemic thrombolysis, a potent and highly cost-effective therapeutic intervention, can significantly reduce the odds of death or dependency. However, dramatic variance currently exists across hospitals. The challenge is to develop new evidence to guide efforts to bridge the evidence-practice gap and improve on treatment delays so that more stroke patients will be eligible for this treatment.
In this context, speedy delivery is a crucial factor in ensuring reperfusion therapy approaches deliver the most benefit per unit cost. Systems based approaches in reducing the time to reperfusion are essential in the delivery of best patient outcomes and best value care. Using a combination of adaptive collaborative workflow embedded within a knowledge translation framework, TEFLON aims to test a system strategy to better deliver high-value care in reperfusion interventions and reduce treatment delays; and therefore, reduce the unwarranted variation in clinical care of acute stroke across two major comprehensive stroke centres in the South West and South East Local Health Districts.
Analysis of the preliminary audit phase has led to a shared development of a TEFLON intervention package. TEFLON has allowed a knowledge translation framework and "champion" based model incorporating highly successful Helsinki and advanced imaging strategies to deliver an effective and generalizable strategy in acute stroke treatment, with potential to be implemented in a wide range of health care platforms. We intend to roll out TEFLON workflow to other tertiary care facilities including peri-metropolitan hospitals.
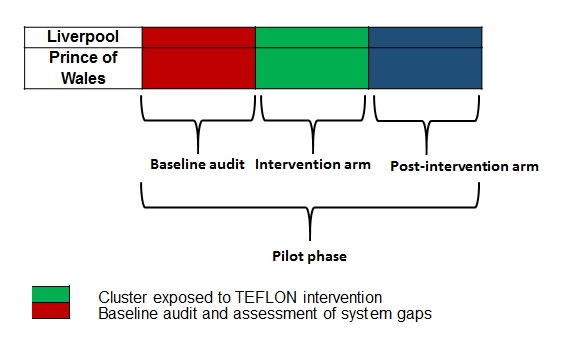
Figure 1. Initial testing of TEFLON implementation, incorporating baseline audit, and intervention arms.
What impact do you imagine the project will have?
This TEFLON model will provide improved efficiency in the delivery of reperfusion therapy across two major hospitals in Sydney, thereby potentially reducing healthcare costs, and improving collaborative workflow, stakeholder satisfaction and quality of life of stroke patients. The TEFLON model may significantly improve the process of care by reducing treating delays and improve stakeholders' engagement with potential for broader uptake as the reperfusion policy.
Our baseline audit phase has led to the recognition of processes and shared development of multidisciplinary collaborative TEFLON intervention package. The package is now being introduced in cycles. The primary outcomes of this initial phase of TEFLON are improvements in the process of care and in reducing treatment delays – specifically, clinically meaningful reductions in door-to-needle or groin time (DNT/DGT) of 20 minutes. This project will provide a robust platform for state-wide reperfusion therapy policy framework and an opportunity for city-wide (Sydney), state-wide (NSW), and potentially national rollout of a system-based reperfusion implementation plan.
My preliminary work on TEFLON has received recognition in the form of First Prize in the Battle of the Mentors at the SWSLHD Health Beyond Research & Innovation Showcase 2018. TEFLON was one of the finalists in the SWSLHD Clinical Quality Awards 2018. The importance of this work gained further traction with oral platform presentation in the category of “Knowledge Translation in Practice” at the 7th Annual NHMRC Symposium on Research Translation held on 27-28 November 2018 at The University of Sydney, Sydney, Australia
How will the project support new collaborations?
I am very passionate about the multicultural diversity we have in South West Sydney (SWS), and the opportunity to be part of this exciting and transformational journey the SWS academic and health precinct is on. SWS has an opportunity to become an exemplary networked comprehensive stroke clinical academic service nationally. However, there is a pressing need to further build stroke research capacity and capability in both SW and SE Sydney to realise this vision.
TEFLON aims to provide an impetus to lift both the research and stroke care improvement profiles, bringing together researchers and clinicians around an education knowledge translation framework and engaging health services management via use of the Institute for Healthcare (IHI) breakthrough series/clinical practice improvement (CPI) approach (noting each hospital has invested significantly in CPI support but often has limited researcher and clinician engagement).
It is noteworthy that the team TEFLON, under my leadership, has engaged across the stroke care continuum – ambulance, ED medicine and nursing radiology/radiography, neurology/stroke medicine and nursing, interventional neuroradiology and hospital service and general management. The teams within the TEFLON partnership are comprised of experts and national leaders in their respective fields who have been firmly committed in the operational aspects to better embed high-quality research in stroke within the hospital stroke care sector.
We have also secured additional seed funding for a community specific awareness project to improve knowledge about stroke and prehospital delay (with A/Prof Dennis Cordato). Research we do is intended to have an impact on our patients in particular and community at large. Our team is committed to further build and potentially expand our collaborative work. It is an exciting time to be in South West Sydney!


