(Sydney, Tuesday 24 July 2018) Globally, more than one in three (39%) people who have injected drugs in the last year are living with hepatitis C infection, according to new research from the National Drug and Alcohol Research Centre and the Kirby Institute at UNSW Sydney.
The research, published today in Addiction, is the first time researchers have estimated the global, regional and national numbers of people who inject drugs that are living with hepatitis C. This work will set the baseline for tracking progress of strategies designed to prevent and treat hepatitis C among people who inject drugs.
“The availability of simple hepatitis C therapies with cure rates greater than 90%, is one of the most exciting advances in medicine in recent decades,” said Associate Professor Jason Grebely from the Kirby Institute, and lead author on the study. “Importantly, recent research from the Kirby Institute has shown that these therapies are very effective at curing hepatitis C among people who have recently injected drugs. We need to expand hepatitis C prevention, testing and treatment strategies among people who inject drugs in order to achieve global hepatitis C elimination.”
In Australia, there are almost 40,000 people who have recently injected drugs living with hepatitis C. However, Australia is one of only four countries worldwide with high coverage of both needle and syringe programs and opioid substitution therapies. “Australia has been an international leader in its response to hepatitis C,” said Associate Professor Grebely. “The fact that hepatitis C treatments are available for all individuals without restrictions based on current or previous drug use means we are likely to achieve the World Health Organisation goal to eliminate hepatitis as a major public health threat by 2030, including among people who inject drugs.”
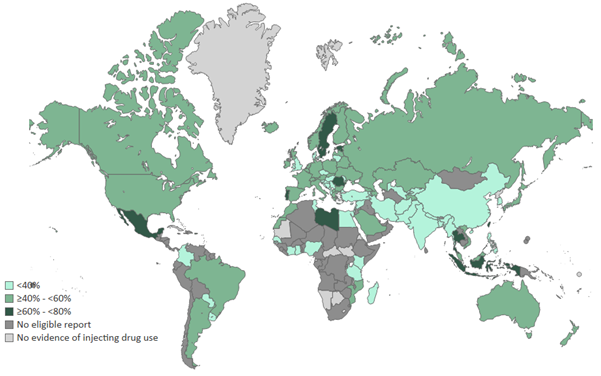
Estimated prevalence of HCV viraemic infection among current people who inject drugs, by country.
According to the new research, among the 71 million people living with hepatitis C globally, 6.1 million people have recently injected drugs. While this only represents 8.5% of all infections, there is a considerable further burden among people with a history of injecting drug use. It is estimated that 25% of all new hepatitis C infections occur among people who inject drugs, as a result of sharing needles and syringes. As such, people who inject drugs are a priority population for hepatitis C elimination efforts.
“Globally, access to harm reduction is poor, with only 1% of people who inject drugs living in countries where needle and syringe programs and opioid substitution therapy are widely available,” said Dr Sarah Larney from the National Drug & Alcohol Research Centre, co-author of the study. “We know these harm reduction strategies are effective in preventing hepatitis C. We must improve our efforts to enhance strategies to prevent hepatitis C infection and reduce the number of new infections.”
The new research reveals that the greatest numbers of people with hepatitis C who have recently injected drugs live in Eastern Europe, East and Southeast Asia, and North America. Globally, half of all people with hepatitis C who have recently injected drugs live in four countries: the Russian Federation, the United States, China, and Brazil.
Judy Chang, Executive Director of the International Network of People Who Use Drugs, said, “it is concerning that over half of all hepatitis C infections among people who have recently injected drugs occur in countries with inadequate coverage of harm reduction services. The global elimination of hepatitis C as a public health threat will not be achievable unless we improve access to harm reduction services, de-stigmatise drug use and drug users, and improve the overall health of people who use drugs.”
Access the full article: https://onlinelibrary.wiley.com/doi/full/10.1111/add.14393
MEDIA CONTACTS
Luci Bamford, Kirby Institute, lbamford@kirby.unsw.edu.au, 0432 894 029
Marion Downey, NDARC, m.downey@unsw.edu.au, 0401 713 850
STAKEHOLDER COMMENT
“We have the tools to eliminate hepatitis C, but we will never reach the World Health Organisation elimination targets unless we prioritize people who inject drugs. Treatment for hepatitis C has been a revolution in medicine: the first ever cure for a chronic viral infection. But we have to get the cure to the people who need it.”
– Michael Ninburg, President, World Hepatitis Alliance
NHMRC Program Grant to conduct research to improve the health of people who use drugs
This research marks the first major output of a collaboration established between the National Drug and Alcohol Research Centre (NDARC) and the Kirby Institute, both at UNSW Sydney. The two institutes were awarded a $9M National Health and Medical Research Council Program Grant to conduct research to improve the health of people who use drugs, with an emphasis on hepatitis C and innovative responses to substance use and related harms. The program grant is led by Kirby Institute Professors Gregory Dore and Andrew Lloyd and Professors Louisa Degenhardt and Michael Farrell from NDARC.



